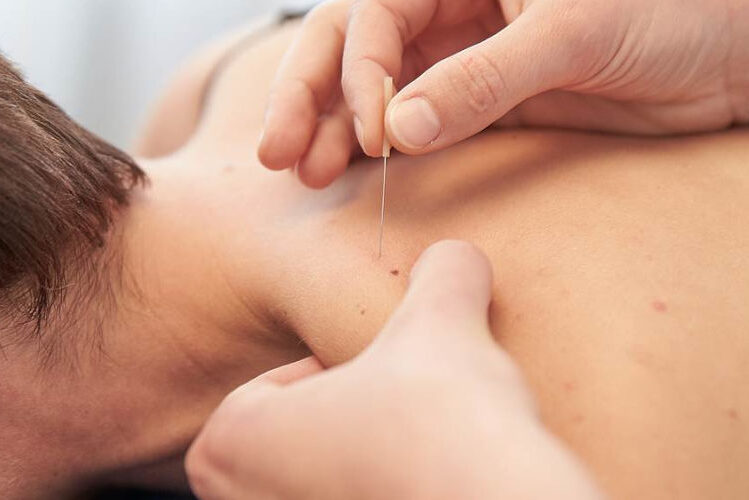
Physiotherapy and Understanding Dry Needling
You may have heard a friend or family member talking about dry needling as part of their care. This treatment technique began in the early 1980’s but has become popular as part of a physiotherapy treatment plan over the past 15-20 years.
Dry needling is an invasive technique where fine needles are inserted through skin into muscles. Trained physiotherapists target areas of tightness and hypersensitivity within muscles. These areas are commonly referred to as Myofascial Trigger Points (MTrPs). In more simple terms – MTrPs are palpable tender spots or knots.
Prolonged tightness in these tender spots can lead to low levels of oxygen called hypoxia. MTrPs can occur from trauma, like muscle contusions or strains, or from chronic overloading during prolonged postures or elevated muscle tension.
Myofascial pain is very common. It has been previously estimated that over 50% of patients presenting to a primary care physician complaining of myofascial pain. Despite this MTrPs are thought to be undiagnosed by primary health care practitioners. This may frequently lead to over-prescription of analgesic medications and a symptomatic, rather than causative treatment approach.
Dry needling of MTrPs may seem similar to Traditional Chinese Acupuncture (TCA). However, TCA is based on treating and balancing a system of meridians or nerve pathways. TCA seeks a balance of energy flow (Yin and Yang Theory) throughout the body. TCA not only aims to treat myofascial pain, but other health concerns such as fertility, allergies, and depression.
The physiological impacts of dry needling are proposed to be lower muscle tone, increased blood flow, and resultant pain relief. Pain relief may also be provided by a release of endorphins in your brain.
The first step in considering dry needling as a treatment approach is accurate patient diagnosis. Second, ruling out contraindications and patients who may be prone to adverse effects from dry needling. If your therapist identifies MTrPs they may offer dry needling as a treatment option. However, dry needling is not for everyone. Using dry needling to treat MTrPs is often uncomfortable. Patients with a needle phobia or those unwilling to experience temporarily increased pain at the treatment site are not good candidates for dry needling treatments. Informed consent must always be provided by the patient prior to treatment.
Patient success with dry needling involves effective communication and trust between patient and therapist. On your first treatment, you may only have treatment one or two MtrPs to gauge your tolerance. Generally, you can expect up to five or six dry needling sessions to see significant improvements in your condition.
As dry needling is only one aspect of patient care. The improvements after therapy must be maintained by an appropriate home program. This could be a combination of stretching, strengthening, and neuromuscular re-education. Meaning patients need to do homework to optimize and ensure their recovery continues.
Dry needling is a treatment option at Progress Physiotherapy. Ask your therapist for more information at (613)-634-1100 or (613) 634-6000. Book an appointment here.
.
Scott Vowles, PT
Scott is a physiotherapist with over 20 years of experience in helping patients achieve their goals.
- Certified Active Release Techniques (ART) provider
- Certified Acupuncture practitioner, Acupuncture Foundation of Canada Institute (CAFCI)
- Certified Functional Movement Screen (FMS) and Selective Functional Movement Assessment (SFMA) provider
- Member of the Orthopaedic Division of the Canadian Physiotherapy Association
- Titleist Performance Institute (TPI) Medical Professional (MP3)
- Former President of the Quinte/St. Lawrence Branch of the Ontario Physiotherapy Association (OPA)
- Former Adjunct Professor of Queen’s University School of Rehabilitation
- Clinical Instructor, Queen’s University School of Rehabilitation